GP Crisis: Australia’s Sicker Patients Forced to Pay the Price for Short Consultations
- Australian patients with chronic illnesses are being forced to pay out of pocket for longer GP consultations, leading to delayed diagnoses and worsening health outcomes.
- 20 peak health bodies are calling for a 40% increase in Medicare rebates for longer GP consultations to address the issue.
- The current system incentivises shorter consultations, leaving patients with complex health needs without the time they need with their GP.
The average patient spends just 20 minutes in their GP’s office, a timeframe doctors say is woefully inadequate to catch subtle signs of illness. For patients with comorbidities or chronic health issues, this standard consultation can barely scratch the surface of their concerns. The consequences are dire: delayed diagnoses, worsening health outcomes, and increased hospitalisations.
The Royal Australian College of GPs (RACGP) is leading the charge, calling for a 40% increase in Medicare rebates for longer GP consultations. “When people can’t afford longer GP appointments, complications and other health issues develop — people get sicker and need expensive hospital care,” RACGP president Dr Michael Wright said.
For patients like Sarah Willits, a 47-year-old Victorian mother of two living with kidney failure, managing her chronic health condition leaves no time in a standard session to discuss other health concerns. “By the time I get through all my physical issues with my GP, time is up,” Willits said. “I would love longer appointments to have the chance for a wellbeing check to get the help I need with related issues.”
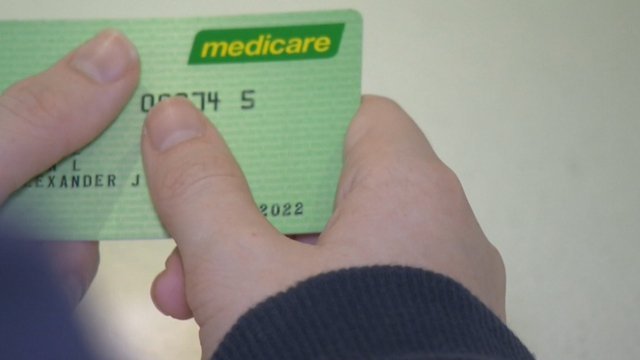
Peak bodies are united in their call for change, citing the critical importance of long consultations for conditions that require timely diagnosis for treatment to be most effective. MS Australia CEO Rohan Greenland said, “Many of the early signs of multiple sclerosis (MS) are invisible or subtle, and timely diagnosis depends on GPs having enough time to recognise symptoms, listen carefully, and refer early.”
Motor Neurone Disease (MND) Australia CEO Clare Sullivan echoed the sentiment, saying reaching an MND diagnosis is “often clinically difficult” and that “access to longer consultations to provide rapid and accurate diagnosis is crucial”. Diabetes Australia CEO Justine Cain said for the two million people with diabetes, a long consultation can “provide critical time to consider a referral to a credentialled diabetes educator or endocrinologists where appropriate”.
Analysis: What This Means for Australia
The knock-on effects of delaying care and diagnoses can be drastic, including an increase in hospital and emergency presentations. Australian Patient Advocacy Alliance CEO Deidre Mackechnie said, “Inadequate management of a chronic condition can result in disease progression to the point of disability, including the need to access the NDIS.” The economic impact is significant, with analysis showing increasing patient Medicare rebates for long GP appointments would deliver more than $338.9 million in annual healthcare system savings.
Security analysts say the current system is failing patients, incentivising shorter consultations that can compromise health outcomes. “The per-minute value of patient Medicare rebates decreases as patients spend more time with their specialist GP. That means, for many people, the sicker you are, the more you pay out of pocket,” the RACGP said.
Industry observers believe the only way to reduce out-of-pocket costs for patients who can’t be bulk-billed is to increase the Medicare rebate patients receive for longer consults. With 20 peak health bodies united in their call for change, it’s clear that the current system is unsustainable. It’s time for Australia to rethink the way we approach GP consultations, putting the needs of patients first.